The vertical height of the upper face (forehead) is classically known as being one-third of the total vertical height of the face. While a long forehead skin distance is described as greater than 10mm of the mid facial height or more than 6.5cms between the eyebrows and the hairline, in the end all that matters is the patient’s perception of it.
Vertical forehead shortening can only be achieved by changing the position of the hairline through two approaches. Hair transplantation is one viable technique that spares a surgical incision and can best artistically lower the hairline without shape limitations. The other approach is a surgical one with frontal hairline advancement. This creates an immediate hairline lowering that has the same hair density and the amount of movement depends on the scalp’s natural elasticity. While effective it has the potential disadvantages of a hairline scar, temporary vs permanent loss of scalp sensation and limits in hairline shaping.
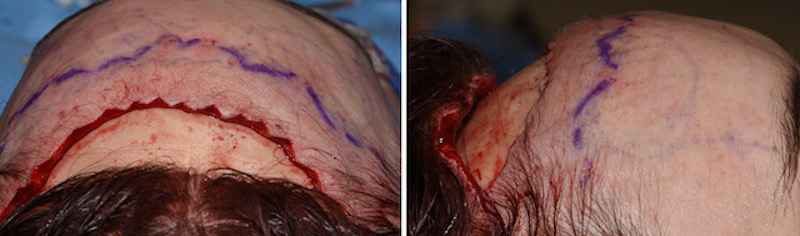
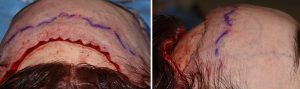
In the February 2019 issue of the journal Plastic and Reconstructive Surgery an article was published entitled ‘Multiplane Forehead Shortening: Sparing the Frontal Muscle and Supraorbital Nerve’. As the title of the paper indicates the goals of the modifications in surgical technique were to better preserve anterior scalp sensation and prevent frontal muscle animation deformities in frontal hairline advancement for forehead reduction. Its modifications consist of a partial thickness incision of the upper forehead tissues which leaves intact most of the galea and the supraorbital nerve branches. A central window of full thickness excision is done through the the subgaleal dissection and tissue elevations are done for scalp mobilization.
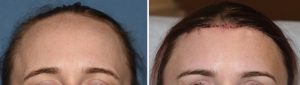
In an impressive 525 patients most of whom were females, this technique was used to create an average 2 cm hairline advancement. Loss of sensation was seen only in the central anterior scalp where the supratrochlear nerve supplies and would have been cut off with the central window. Acceptable scars were obtained in 85% of teh patients by six months after the surgery. After surgery alopecia was seen in only two patients. A natural movement across the forehead and scalp was seen in all cases.
Dr. Barry Eppley
Indianapolis, Indiana