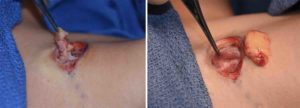
Background: The placement and removal of a tracheostomy always results in some degree of neck scarring. The longer the tracheostomy is in place, the more significant this scarring will be. The characteristics of the trach scar are classic and include a wide and depressed scar that is often associated with a visible inward movement when swallowing.
One of the key anatomic features of the trach scar is the crater-like appearance to it. The pressure of a plastic tube against the tissues of the neck ultimately causes some loss of subcutaneous fat around the tube site. The longer the tracheostomy tube is in place the more significant this fat loss will be. Thus when the tube is removed the open wound will heal but the surrounding tissues will be depressed inward as a result of the fat loss.
The other anatomic feature of the trach scar is an inward contraction seen when swallowing. This occurs due to the loss of fat but also from the development of a scar that extends from the surface of the skin down to the actual trachea. When the trach tube is removed secondary healing creates this scar band. When one swallows the movement of the trachea is transmitted through the scar band up to the skin surface.
Case Study: This 21 year-old female had a central neck scar from a tracheostomy tube that was removed ten years earlier. It had been in place after having it for five years due to severe reactive airway disease as a child. This left her with a bothersome vertically-oriented central neck scar that was depressed inward, had surrounding hyperpigmentation and pulled inward when swallowing.
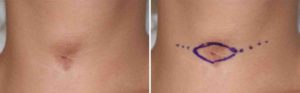
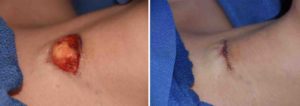
While all trach scars will always be a scar, a scar revision should end up making it look less noticeable. One of the key features of achieving that goal is to have a flat outer contour and a scar that remains stable with swallowing. The use of a dermal-fat graft recreates the principal missing element of a trach scar…lost fat. Replacing the lost fat improves the scar contour and acts as a buffer from the skin surface and the deeper underlying trachea.
Highlights:
1) Depressed and retracted trach scars require adequate release from the tracheal ring.
2) Interpositional fat grafting between the skin and the underlying trachea helps create a smooth outer skin contour and prevents visible skin retraction with swallowing.
3) Small dermal-fat grafts survive very well in the trach scar neck site.
Dr. Barry Eppley
Indianapolis, Indiana