Background: Enlargement of the breast tissue in a teenage or adult male, well known as gynecomastia, is a challenging aesthetic chest problem. It is comprised of several components including the amount of breast tissue, the size of the areola, and the position of the nipple-areolar complex on the anterior chest wall. Much of the focus of gynecomastia surgery, understandably, is on the reduction of the size of the breast mound whether it is throughout the whole chest or just limited to around the nipple-areolar complex.
Reduction of the breast tissue in gynecomastia can be done by either liposuction, direct excision through a lower areolar incision or both. Which of these approaches is best is determined by the size and quality of the breast tissue. Male breast tissue can be simplistically divided into ‘soft’ and ‘hard’ types. Hard breast tissue is known as glandular tissue and is very firm, lump-like and largely relegated to underneath and around the nipple-areolar complex. Soft breast tissue is largely comprised of fat with some fibrous tissue, known as fibrofatty tissue. It can occupy the entire chest or be an extension beyond the zone of glandular tissue underneath the nipple.
As a general rule, hard gynecomastia responds best to direct excision as it needs to be cut out. Soft gynecomastia can be extracted without excision by liposuction. Many gynecomastia conditions require both methods given the mixed hard and soft tissue make-up. If glandular tissue is not recognized before surgery, residual lumps or areolar fullness may be left behind by liposuction.

Case Highlights:
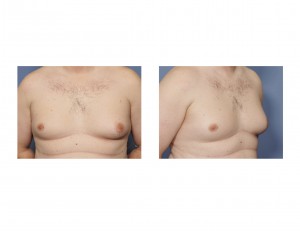
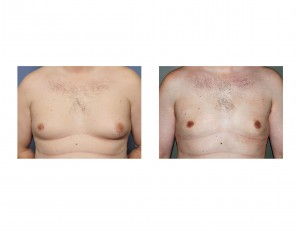
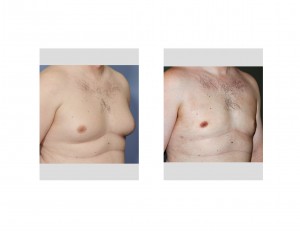
1) Male gynecomastia responds to different treatment approaches based on the type of breast tissue and the size and position of the nipple-areolar complex.
2) In ‘soft’ forms of gynecomastia without significant glandular tissue, liposuction can be very effective at chest contouring/reduction.
3) Liposuction of gynecomastia, specifically using Smartlipo, can be done with very small incisions and without the need for drains.
Dr. Barry Eppley
Indianapolis, Indiana


