I get a lot of inquiries regarding the use of hydroxyapatite(HA) for facial augmentation. Some requests are for whether it will work for their facial augmentation needs. Others are with concerns about indwelling HA materials at various craniofacial implantation sites. Depending upon what you read and whom has written it, the advisability and safety of HA facial augmentation can be positive or negative.To provide some clarity to the use of HA, I have written the following brief review on the topic.
Hydroxyapatite is a calcium phosphate materials that is similar to bone (HA is 70% of the inorganic mineral in bone) and has bioactive and osteoconductive properties. Calcium phosphate materials come in a very wide variety of forms such as cements, blocks, granules and coatings and are used in many medical and dental applications. Such calcium phosphate synthetic materials come in two common forms, hydroxyapatite and tricalcium phosphate. (TCP) These two materials are often confused and are in appropriately used interchangeably. Hydroxyapatite is best thought of as non-resorbable while TCP is resorbable. To matters somewhat more confusing there are even combined biphasic HA-TCP composites for clinical use.
It is important to realize that the term, hydroxyapatite, is really a generic one. There are many different forms of synthetic HA based on its porosity, density and how it is processed. Because it can be made fairly inexpensively there are many manufacturers around the world. Their similarities and differences are impossible to know from a surgeon and patient standpoint. Thus it would be presumptous to assume they all behave the same biologically or are even equally safe.
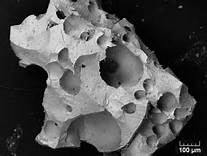
There is extensive clinical evidence that hydroxyapatite granules are very safe, well tolerated and exhibit substantial bony ingrowth/overgrowth. I have seen and treated many HA granule facial augmentation patients and have seen their results both preoperatively by 3D CT scan and intraoperatively for removal/adjustment. I have always been impressed by the bony growth in and around the granules. Inflammatory reactions and bone destruction/degradation have never been observed.
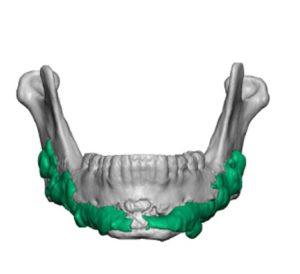
In conclusion I like hydroxyapatite granules for onlay facial augmentation for its safety, effectiveness and method of application. But its aesthetic effects are often problematic and severely limits its use. For small craniofacial augmentation sites it has a role but patient selection is critical. It works best when it is not asked to do too much.
Dr. Barry Eppley
Indianapolis, Indiana



