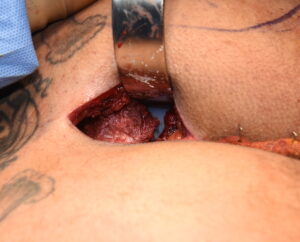
Background: Implants are the assured permanent method of buttock augmentation even though they are far less commonly performed compared to BBL surgery. (fat injections) Patients typically seek out buttock implants because they do not have adequate fat stores to harvest for BBL surgery or they have received inadequate BBL results. The present debate with buttock implants is whether they should be placed on top of or inside the gluteus maximus muscle. (subfascal vs intramuscular) This decision is driven by the size of the buttock increase desired, surgeon preference/experience and the patient’s tolerance for complications.
By far the use of the intramuscular position for buttock implants has fewer potential complications than the subfascial location on the top of the muscle. While it is a far more difficult procedure to create the implant pocket where there is not a natural tissue plane, its deeper position in the buttock tissues is the key for lowering complications. The risks of infection, the development of various types of fluid collections (hematoma, seroma) and shifting of implant position long term after surgery are all lowered by being in a well vascularized and tighter tissue pocket.
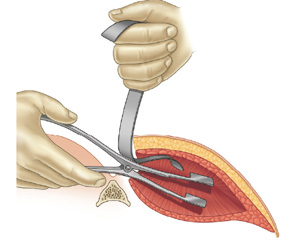
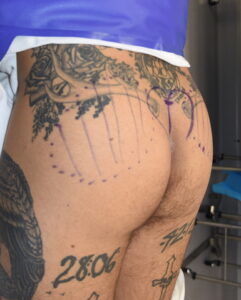
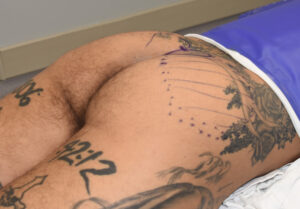
Case Study: This patient specifically desired intramuscular buttock implants of which the size discussed was in the range of 300 to 400ccs. It was agreed that whatever the size of the implant that could be placed with good muscular closure over it would be used. While maximal implant size was desired, an implant size that fit comfortably in the intramuscular pocket takes precedence.
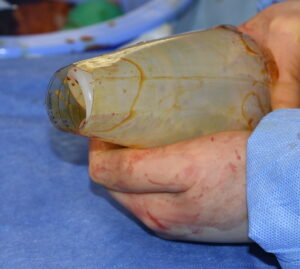
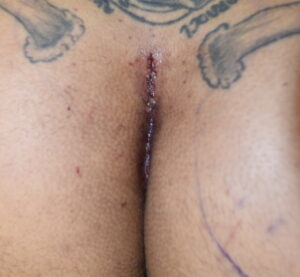

Case Highlights:
1) Various types of non-female patients undergo buttock enhancement surgery, much less frequently than in females, but with outcomes that are just as successful.
2) The intramuscular buttock implant placement technique is most ideally suited for those patients who prefer an improved shape over a large increase in buttock size.
3) A midline intergluteal incision is preferred for intramuscular buttock implants with emphasis on closure of re-establishing the depth of the intergluteal cleft.
Dr. Barry Eppley
Indianapolis, Indiana