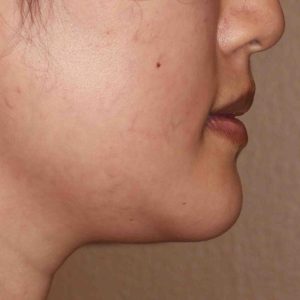
Background: While a sliding genioplasty may be an autologous procedure rather than an implant-based method of chin augmentation, it is still susceptible to the risks of the need for aesthetic revision. The chin may have been advanced too far forward for the patient’s aesthetic desires or time has determined that getting back closer to their preoperative chin shape is more preferred. Either way the chin bone can be recut and returned partially or fully to the preoperative position.
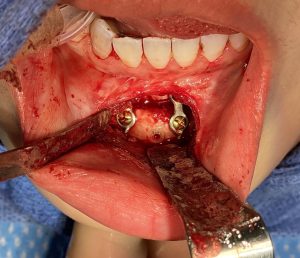
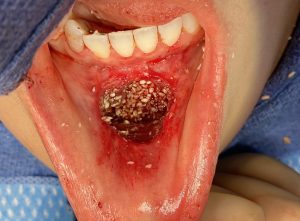
One of the misconceptions of secondary bony genioplasties is that it may not heal well if cut again. That is not true and is a misunderstanding of the anatomy of the chin. A sliding genioplasty is a pedicled bone flap which means, while the tissues are removed from its front surface to perform the osteotomy cut, the soft tissues and the blood supply they provide remain intact at the inferior and posterior bone surfaces. Thus the chin maintains a healthy blood supply and no matter how many times the osteotomy line is cut the bone has enough blood supply to heal again.
Another misconception is that if the bone is partially or fully reversed the surrounding soft tissues will return to their preoperative shape. This is not anymore true than if you remove a chin implant the soft tissue chin pad snaps back to where it was. The soft tissue expansion effects are different in a sliding genioplasty versus a chin implant however. With a chin implant removal can result in some ptosis where the expanded soft tissue pad hangs off of the front surface of the bone a bit. Conversely in a sliding genioplasty the excessive soft tissue appears in the submental region as a fullness. This can be concurrently or secondarily managed by liposuction or a submentoplasty procedure.
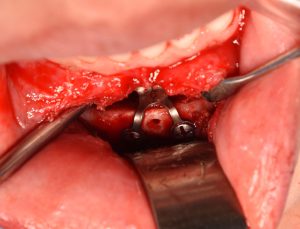
While one should try and avoid having to cut the chin bone more than once, it can be safely done with a very low risk of poor healing. (non-union) This would be particularly true when it is a genioplasty reversal since the original bone thickness is being partially or fully restored.
While the bone may heal uneventfully there may be some ‘new’ soft tissue excesses that appear in the submental region. While in the beginning the submental fullness is definitely swelling and a small fluid collection, over time if any residual fullness exists it is the stretched out neck tissues from the original advancement being pushed back with the bony reversal. This may require secondary management with liposuction or even a submentoplasty procedure.
Case Highlights:
1) A sliding genioplasty can be partially or fully reversed without the risk of developing a bony non-union.
2) The same osteotomy line is used for the secondary genioplasty which is less thick the original chin bone in most cases.
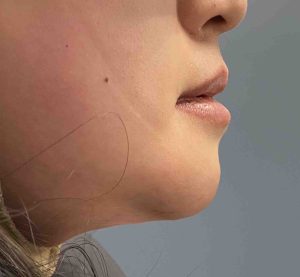
3) When the chin bone is partially or fully reversed there will almost always be the development of increased submental fullness…even if it did not exist before the original sliding genioplasty.
Dr. Barry Eppley
World Renowned Plastic Surgeon