The intergluteal cleft, more commonly known as the ‘crack’, is the attached skin that forms a groove between the two buttocks. It is very similar to the breasts with the attached skin to the sternum forming a cleavage line in the chest between the breasts. The interglueal cleft is approximately 9 to 11 cms long from the top of the visible cleft at the sacrum down to just above the anus.
The intergluteal cleft is a normally innocuous anatomic structure that is paid little attention. But in buttock implant surgery this is the site of the incision to access both buttocks. In so doing it is possible to adversely affect the shape of the intergluteal cleft. The cleft exists because the skin is firmly attached down to the sacral bone with the aid of the sacrocutaneous ligament. Making an incision through or around it risks losing the ligamentous attachment and resulting in webbing or loss of visible separation between the two buttocks.
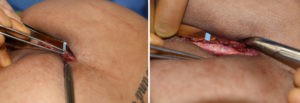
Besides preserving the aesthetics of the intergluteal cleft after the placement of buttock implants, creating a firm midline closure also resists the most common complication of this type of buttock surgery….postoperative wound dehiscence. Due to the shearing forces to which the midline cleft from is exposed from normal activities, some degree of wound separation almost always occurs. Firm fixation of the two buttock incisions to the dermal skin island/ligament helps lessen the severity and occurrence of postoperative wound separation.
Dr. Barry Eppley
Indianapolis, Indiana


