Many parts of the body suffer sagging or loose skin from the effects of aging and gravity. The tissues above moveable extremity joints (knees and elbows), however, has the added influence of motion across the joint with flexion to an arc of up to 120 degrees. As a result the stretching of the soft tissue over the bony joint contributes to loose skin and wrinkles when the extremity is extended.
Such an effect caused by gravity, aging and joint flexion affects the knee. Above the knee cap (patella) a crescent-shaped tissue redundancy can appear. This can be aesthetically disturbing in some women as the knee is very visible in shorts and many skirt styles. This suprapatellar mound of tissue have been treated by a variety of different modalities with very limited success. While liposuction can reduce its fullness this often only results in a deflated appearance and further tissue wrinkling/folds. In some patient it even makes its appearance worse. Non-surgical skin tightening devices and fat reduction methods offer limited to no visible improvement.
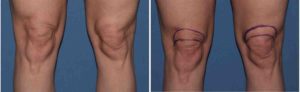
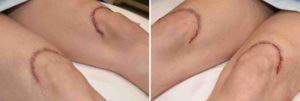
While very effective the issue with the knee lift is the resultant scar and how well it heals. Most heal with a very fine line and an acceptable scar as the aesthetic tradeoff. But the risk of adverse scarring remains and the potential secondary need for a scar revision procedure.
Dr. Barry Eppley
Indianapolis, Indiana


