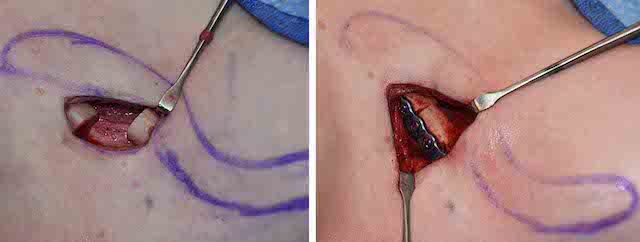
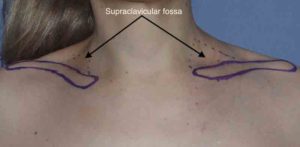
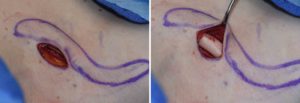
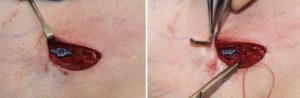
Shoulder feminization surgery reduces the bideltoid width through shortening of the length of the clavicles. While this is a straightforward concept as the lone horizontal bone on the body is the clavicle, doing so in an aesthetic manner requires several key steps to ensure an effective result that proceeds to uncomplicated bone healing and minimal scarring. Key steps are incision placement, amount of bone resection, bone stabilization and wound closure.
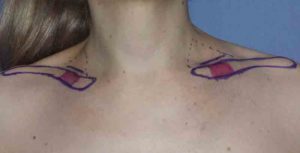
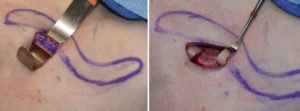
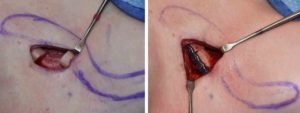
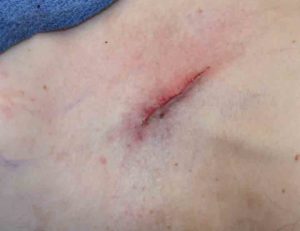
By adhering to these key maneuvers in the procedure a successful aesthetic outcome can be achieved with a low rate of secondary scar revision or need for plate and screw removal.
Dr. Barry Eppley
Indianapolis, Indiana