The Impact of Clavicle Reduction on Body Proportions
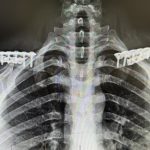
Clavicle reduction osteotomy is an effective procedure for reshaping wide shoulders. By removing a segment of the clavicle bone, the distal shoulder is drawn inward toward the more stable sternal segment. This not only decreases bideltoid width but also softens the square appearance of the shoulders, creating a more tapered upper torso. How Shoulder Narrowing Read More…