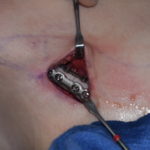
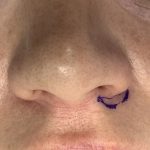
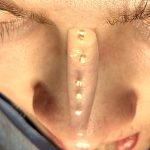
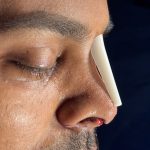
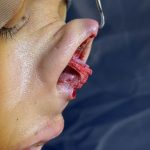
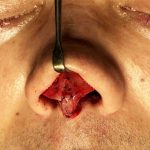
Secondary Dorsal Implant After Inadequate Rib Graft Augmentation Rhinoplasty
Nasal dorsal augmentation involves increasing the height and/or improving the contour of the nasal bridge (dorsum). It is a common component of rhinoplasty, particularly in patients with a low or flat nasal bridge or an irregular dorsal contour. Common Indications Low nasal bridge (common in many Asian, African, or revision rhinoplasty patients) Saddle nose deformity Read More…