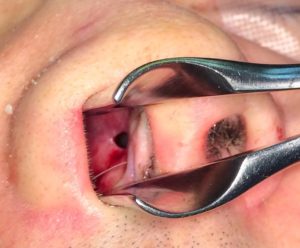
While not all septal perforations are symptomatic or need repair, when they do they are very challenging to do successfully. The many methods described for septal perforation repair from synthetic buttons to grafts, and their varying rates of success, speak to this challenge.
In the November 2016 issue of JAMA Facial Plastic Surgery, an article was published entitled ‘Use of Costal Perichondrium as an Interpositional Graft for Septal Perforation Closure’. In 51 nasal septal perforation patients, the use of costal perichondrium as an interpositional graft with bilateral mucosal flaps was used for the repair. Forty-four (44) of these patients actually underwent closure with this technique which was successful in 42 patients (95%) over an 18 month followup period. Regardless of the septal perforation size treated, costal perichondrium as an interpositional graft aided in the rate of successful closure of the treated septal perforations.
While the technique and experience of the surgeon should not be minimized in the treatment of the septal perforation problem, what is it about costal periochndrium that may make it better than other autologous or allogeneic grafts? Since it requites a small chest incision to harvest it had better have some favorable biologic characteristics.
Costal cartilage is a composite structure composed of cartilage surrounded by a dense tendon-like perichondrium. Costal perichondrium is very different than nasal perichondrium because it is much thicker as it provides some mechanical benefits to the ribcage. Studies have shown that it adds up to 50% more resistance to bending forces across the costochondral junction. This stoutness means it is thick, can hold sutures if needed and be more quickly revascularized than thinner fascial or thicker cadaveric dermal grafts. This means that it may hold up well even if the mucosal flaps break down.
Dr. Barry Eppley
Indianapolis, Indiana


