While scars have a negative connotation due to the imperfect appearance of the skin, they are a normal result of most injuries and surgeries. This is part of the wound healing process and their appearance (or perpetuation) is the expected result of this dynamic process. It is only deviations from normal wound healing, hypertrophic scars and keloids, that should be considered abnormal.
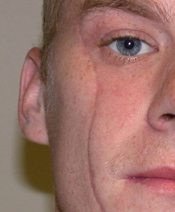
Conversely, keloids extend beyond the confines of the original wound (mushrooming from the wound edges) and are often associated with ongoing growth. They may stop growing but many do not. It is this progression in size that is the hallmark of their behavior. They often cause pain and other symptoms such as itchiness. This is due to the tight scar tissue and a sign of ongoing growth. They may also be a family history of keloids due to a genetic inheritance. They are often associated with traumatic wounds such as ear piercings, tattoos and burns.
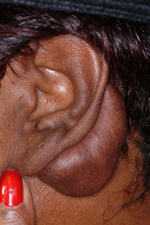
Combining some recurrence prevention strategy with keloid excision is standard and most commonly is the injection of steroids along the wound edges. This is best done before surgery to get some regression of the keloid and then the excision is performed. At the time of excision the wound edges may be injected with steroid followed by repeat injections every several weeks after surgery for a few intervals. This is far more successful that just excising a keloid alone but is still associated with a near 50% recurrence rate.
For the refractory keloid, radiation therapy is the one known alternative approach that is often better than steroids. It is combined with scar revision and is started immediately, even on the day of surgery. It is known as low dose radiation and, while there is no standard dosing regimen, most patients receive between 1500 and 2000 rads over several sessions done daily for the first week after the surgery. This radiation-induced disruption of collagen synthesis at its inception has the best chance of preventing new keloid formation although it is not foolproof and recurrences have been known to recur .
Dr. Barry Eppley
Indianapolis, Indiana


