Short answer: yes, it can—but it’s one of several factors, and not usually the dominant one.
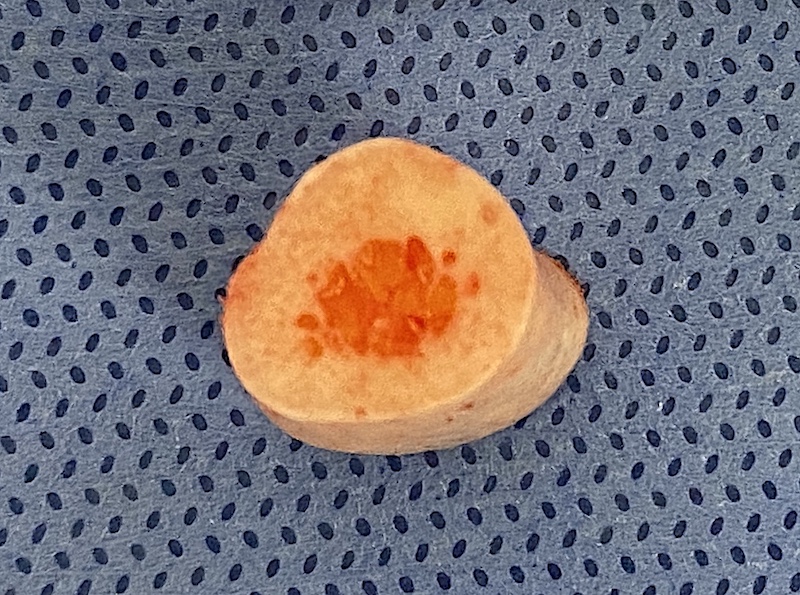
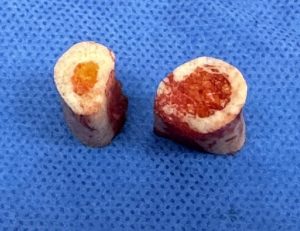
The “marrow space” (intramedullary canal) of the clavicle plays a role in healing because bone repair depends heavily on blood supply and available progenitor cells, both of which are tied to the marrow environment.
Here’s how it matters:
1. Blood supply and biology
- A larger or well-preserved marrow space generally means better endosteal blood flow and more marrow-derived stem cells.
- These contribute to callus formation and remodeling.
- If the canal is very narrow, sclerotic, or compromised (e.g., from prior injury or stress), the biologic contribution may be reduced.
2. Surgical technique interaction
- With intramedullary fixation, canal size directly matters:
- A narrow canal can make fixation more difficult or less stable.
- Over-reaming (if done) can disrupt endosteal blood supply.
- With plate fixation (more common in clavicle fractures):
- Healing relies more on periosteal blood supply, so marrow space is less critical.
3. Fracture pattern and stability
- Healing is more strongly influenced by:
- Stability of fixation
- Degree of comminution
- Soft tissue preservation
- Even with a small canal, good mechanical stability usually leads to solid healing.
4. Patient-specific factors
- Age, smoking, metabolic health, and vascular status often outweigh canal size in importance.
Bottom line (Fracture – Specifc)
- The size/quality of the clavicle’s marrow space can influence healing biology, particularly for intramedullary techniques.
- But in most real-world cases—especially with plate fixation—mechanical stability and periosteal blood supply are far more important determinants of healing than canal size alone.
In clavicle reduction osteotomies, the relevance of the marrow space (intramedullary canal) becomes a bit more specific—and somewhat more important than in routine fracture fixation, but still not the primary driver of healing.
Here’s how it plays out in this setting:
? 1. Biology at the osteotomy site
- An osteotomy is a controlled surgical fracture, so healing relies on the same principles:
- Periosteal blood supply (dominant in clavicle)
- Endosteal/marrow contribution (secondary but helpful)
- If the marrow canal is:
- Patent and vascular ? contributes progenitor cells and internal blood flow
- Sclerotic or narrowed (common in malunions/nonunions) ? reduced biologic activity
? In revision cases or long-standing deformities, the canal is often partially obliterated, which can slightly impair healing potential. But this is rarely the case in the clavicle reduction patient
2. Canal size & surgical technique
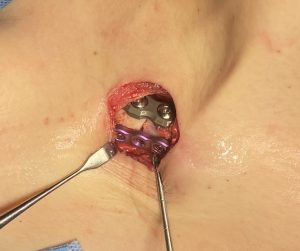
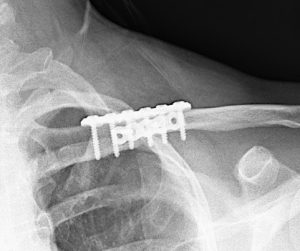
In reduction osteotomies, intramedullary fixation devices are not currently used. Most clavicle osteotomies are fixed with plates, meaning:
- Healing is primarily periosteal and external callus–driven
- The marrow space becomes less critical than:
- Rigid fixation
- Compression across the osteotomy
- Preservation of soft tissues
Fixation matters more than
?? 3. Where marrow space does matter clinically
It becomes more relevant in:
- Atrophic nonunion corrections
- Revision osteotomies
- Prior hardware or multiple surgeries
- Situations where you’re relying on biologic augmentation (e.g., bone grafting)
In these cases:
- A poor or obliterated canal ? often prompts:
- Opening the canal
- Adding autograft (iliac crest)
- Enhancing biology deliberately
Bottom line (osteotomy-specific)
- Marrow space condition modulates the biology, especially in revision or compromised bone.
- But successful healing after clavicle reduction osteotomy still depends far more on:
- Stable fixation (usually plate + compression)
- Good osteotomy technique
- Preserved periosteal blood supply
Dr Barry Eppley
Plastic Surgery