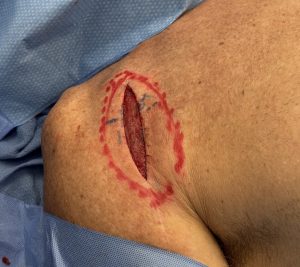
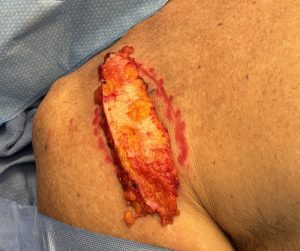
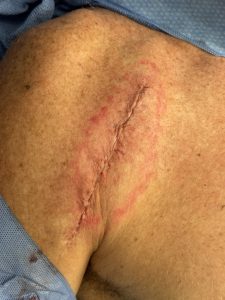
Custom deltoid implants can be considered for visible deltoid/shoulder hollowing after shoulder replacement, but they are contour-restoration devices, not functional muscle replacements.
Key points:
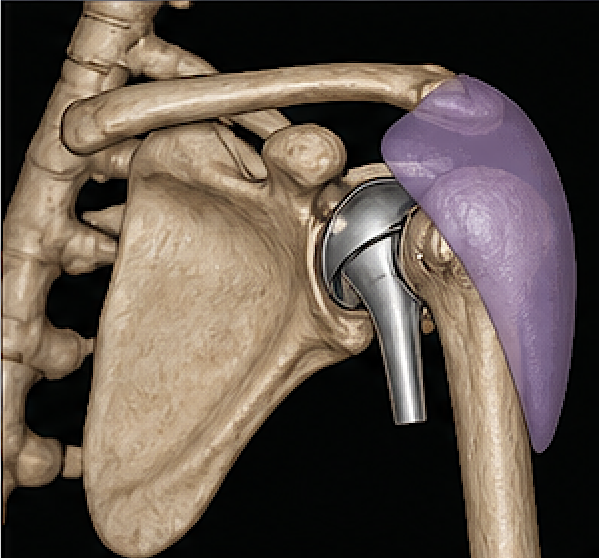
- After reverse shoulder arthroplasty, deltoid quality matters because the deltoid becomes the main elevator of the arm. Deltoid atrophy or nerve injury can affect function.
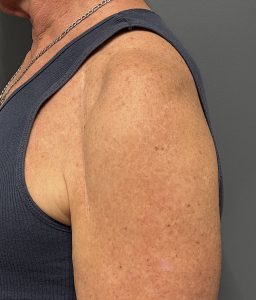
- A solid silicone custom deltoid implant may help restore the rounded shoulder contour when the atrophy is stable and localized. This is mainly aesthetic/symmetry reconstruction.
- It will not restore deltoid strength if the muscle/axillary nerve is deficient.
- With a prior shoulder arthroplasty, the major added concerns are:
- proximity to prosthetic hardware
- infection risk
- scarred surgical planes
- need to avoid deltoid compromise
- confirming the shoulder replacement is stable and not infected
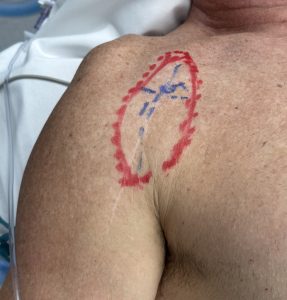
For a post-arthroplasty patient, I’d generally favor a custom low-profile deltoid contour implant placed superficial to the deltoid/fascial plane, designed to camouflage the hollow without interfering with the shoulder prosthesis. But when only a thin soft tissue cover lies over the incision line direct implant placement underneath it is not advised. Soft tissue volume restrodation is needed by fat grafting. Dermal-fat grafting is needed to create increased soft tissue thickness, particularly at the anterior deltoid-pectoral junction prior the placement of the implant. This is a superior approach to fat injections in effectiveness.
Case Example
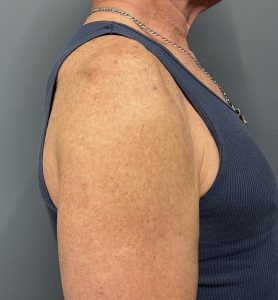
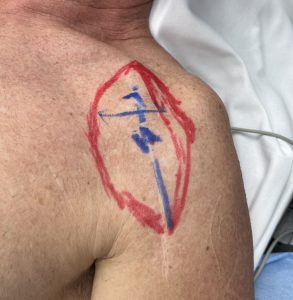
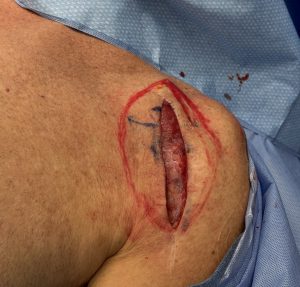
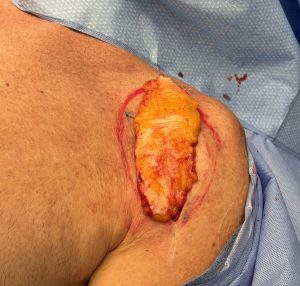
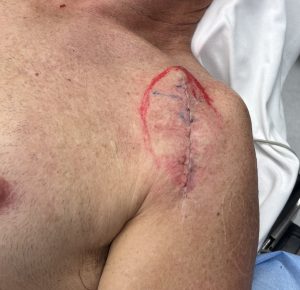
Discussion
Large dermal-fat grafts can be a useful option for correcting shoulder soft-tissue asymmetries, but they’re not commonly discussed in the same way as facial or breast applications—so the indications and limitations matter a lot.
Conceptually, you’re using a composite graft (dermis + attached fat) to provide:
- Volume (fat component)
- Structural stability and resistance to resorption (dermis component)
That makes them different from standard lipo-fat grafting, especially in areas like the shoulder where:
- Skin is thicker
- Motion is high
- Shear forces can compromise pure fat graft take
When they make sense in the shoulder
Large dermal-fat grafts are most appropriate when the asymmetry is:
- Focal and contour-based (not diffuse volume deficiency)
- Associated with soft tissue deficiency, not just muscle imbalance
- Post-traumatic or post-surgical (e.g., deltoid contour loss, clavicular prominence, AC joint region irregularity)
- Stable defects, not evolving conditions
They can also be useful in:
- Congenital asymmetry (e.g., mild Poland-like presentations without major muscle absence)
- Implant camouflage situations (less common in shoulder vs chest)
Advantages over fat grafting alone
- Lower resorption variability (dermal scaffold helps)
- More predictable shape retention
- Better for defined contour defects rather than generalized volume
- Less dependent on perfect recipient bed vascularity (to a degree)
Limitations / challenges
This is where reality pushes back a bit:
- Size constraints
- “Large” grafts risk central necrosis if they exceed revascularization capacity
- Shoulder region is not as forgiving as face
- Contour visibility
- Shoulder skin is relatively thin over bony landmarks ? graft edges can show if not feathered well
- Mobility
- Deltoid motion ? shear ? risk of partial loss or fibrosis
- Donor site morbidity
- Typically gluteal fold or lower abdomen
- Large grafts = noticeable donor scar
- Fixation
- Requires secure pocketing and sometimes suturing to prevent migration
Technical considerations
- Layered placement rather than one thick block when possible
- Meticulous pocket creation (subfascial vs subcutaneous depending on defect)
- Immobilization post-op (often underappreciated for shoulder cases)
- Consider combining with:
- Fat grafting (hybrid approach) for edge blending
- Local tissue rearrangement if skin deficiency exists
Alternatives (often more practical)
Depending on the defect, these are frequently used instead:
- Autologous fat grafting (serial sessions)
More adaptable for broad asymmetry - Silicone or custom implants
Rare in shoulder, but possible for structural deficits - Muscle flaps (e.g., latissimus, local advancement)
For larger or dynamic defects - Allograft dermal matrices
Occasionally used, but less volumetric than autologous dermal-fat
Bottom line
Dermal-fat grafts can work well for moderate, well-defined shoulder contour defects, especially when you need more structural persistence than what fat injections can achieve.
Dr Barry Eppley
Plastic Surgeon