The temporomandibular joint (TMJ) creates the articulation between the lower jaw and the skull. It allows the mandible to open and close and creates the capability for the only moveable bone in the entire craniofacial skeleton. The TMJ is about the size of one’s thumb and is composed of a ball (condyle of mandible) and socket. (glenoid fossa of the temporal bone) Hence the term, temporomandibular joint)
Like all joints in the body, the TMJ is equally prone to degenerative changes by age-related osteoarthritis and the more aggressive immunologic disorder of rheumatoid arthritis. When significant condylar erosion has occurred, the joint may need to be rebuilt. This can be done by either an autologous approach using costocbondral rib grafts or the prosthetic approach of a total TMJ joint replacement system.
The TMJ joint replacement system borrows from the orthopedic joint replacement world with a metal condylar prosthesis and a high density polyethylene-based glenoid fossa insert. This glenoid fossa implant is attached along the temporal bone in front of the ear and has a cup shape that sits in and replicates that natural bony glenoid fossa. The metallic condylar prosthesis then fits into the fossa implant, recreating the ball and socket of the TMJ.
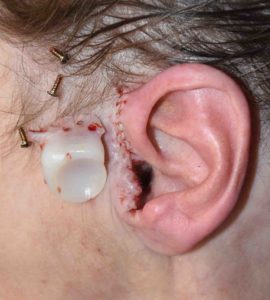
This 73 year-old female had a total TMJ replacement done 15 years for her severe rheumatoid arthritis and jaw dysfunction. Over the past year she developed some intermittent pain and drainage from the left ear canal. Multiple ENT physicians examined her ear and could not find any source for her ear drainage and pain.
Dr. Barry Eppley
Indianapolis, Indiana


