Here’s how it’s typically approached and what makes it unique:
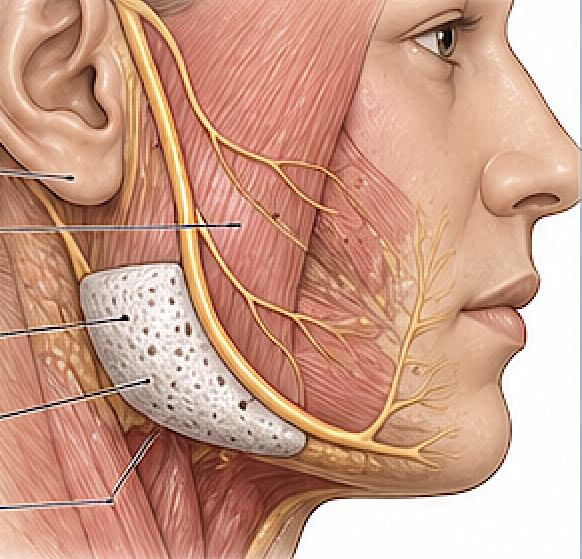
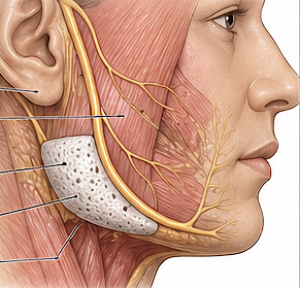
Key Anatomical Challenges (Jaw Angle)
- Facial artery (most critical risk)
- Masseter muscle (implant often partially embedded)
- Pterygomasseteric sling
- Thick periosteum and dense soft tissue
- Limited exposure compared to chin/cheek
Surgical Approach
1. Incision Choice
Most commonly:
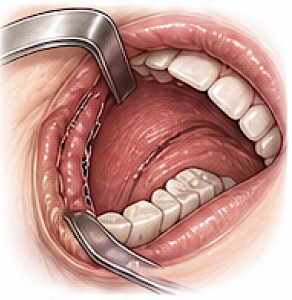
- Intraoral (posterior vestibular incision)
- Avoids external scar
- More difficult exposure
- Can not see the bottom of the implant…where all the risk issues reside
Less commonly:
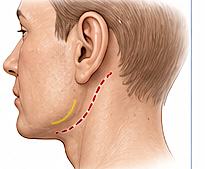
- External (submandibular/retroauricular)
- Used in:
- When such an existing incisions exists as out was initially placed that was
- Better preservation of masseter muscle/ptergo-masseteric sling
- Need for wide exposure along the bottom of the implant
- Used in:
2. Subperiosteal Elevation
- Elevation along:
- Mandibular ramus ? angle ? posterior body
- Key principle:
- Stay on bone initially to avoid muscle disruption/ injury
- Easiest tissue plane to elevate since no bone ingrowth occurs
3. Identification & Protection of Masseter Muscle
Techniques:
- Sharp dissection on external and bottom surface of implant
- Avoid:
- Aggressive inferior blind dissection on bottom of implant as the facial artery crosses the inferior border of the mandible at the angle-body junction
- If external approach:
- Better visualization of the underside of the implant and ligation of the facial artery should njury to it occur
Risk:
- Temporary severe bleeding, controlled by ligation
- Masseteric muscle dehiscence if it did not exist before
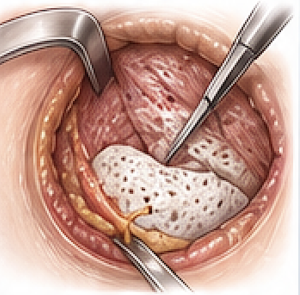
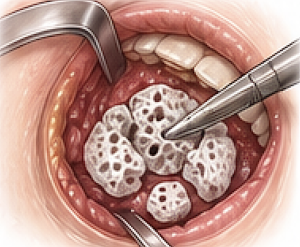
4. Piecemeal Implant Removal (Almost Always)
- Medpor Jaw angle has thick and highly integrated tissue ingrowth
- Technique:
- Dissect free in segments and sequentially remove.
- Only remove what you know is adequately dissected free and can be visualized
- Each implant segment removed allows more oif the implant to be seen and safely removed.
- Tools:
- Sharp elevators
- Needle point electrocautery
- Osteotomes
5. Screw Removal
- Almost all Medpor jaw angle implants will have multiple screws for fixation
- If done intraorally remove implant around the screws to expose their long threaded shaft and then turn them out by a needle holder
- If done externally use a screwdriver and remove in conventional manner
6. Hemostasis in a Vascular Field
- Masseter + ingrowth = significant bleeding
- Use:
- Electrocautery
- Maintain:
- Clear visualization at all times
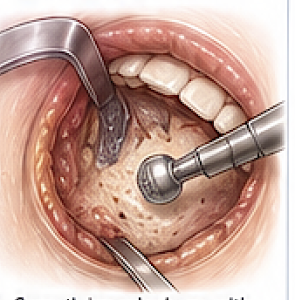
7. Bone and Contour Management
After removal:
- Common findings:
- Irregular angle contour
- Mild resorption
- Management:
- Large bony overgrowths can be removed
- Imprint of the bone is not necessary to treat
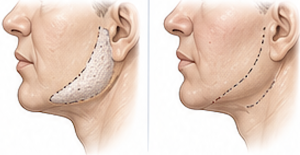
6. Soft Tissue Considerations
- After implant removal:
- Loss of projection at angle
- Possible soft tissue sagging
Management options:
- Await secondary assessment after full healing at which time options include::
- Fat grafting
- New implant
- Jowl-neck tuck
0. Drain Placement (Often Recommended)
- Due to:
- Dead space
- Muscle dissection
- Helps prevent:
- Hematoma
- Seroma
Unique Risks in Jaw Angle Medpor Removal
1. Masseter Muscle Dehiscence
- Jaw angle soft tissue contour deformity, may take months to fully see
- May be worse after implant removal if it existed before
- Can be prevented or treated with an external approach only
2. Residual Implant Fragments (rare)
- May be intentionally left if adherent to artery
- Most commonly small retained implant pieces occur because they could not be seen or found
3. Prolonged Swelling
- Jaw angle region swells more and persists longer than the chin and cheek areas
Practical Surgical Philosophy
- Try and remove every implant fragment
- Be prepared to fragment for removal, don’t avulse
- Preserve masseter muscle as much as possible
- Be aware of the facial artery location and dissect accordingly
Compared to Other Medpor Locations
Jaw angle removal is:
- Much harder than chin or cheek
- More challenging than initial implant placement
Dr Barry Eppley
Plastic Surgeon