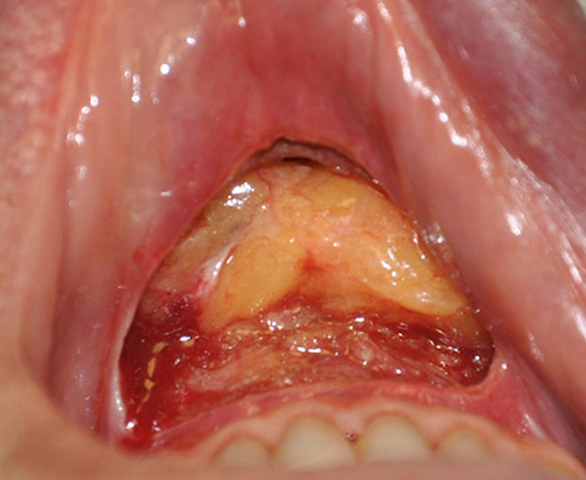
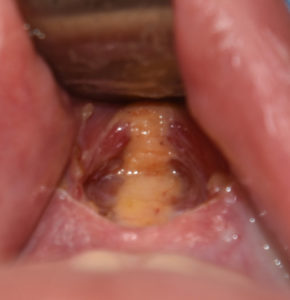
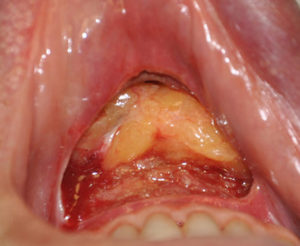
In every intraoral dissection of the chin, the mentalis muscle is encountered and transected to some degree. In most cases the surgeon’s goal is to leave the actual muscle attachment to the bone intact (its point of origin) so that it can serve as reattachment area during closure. While this reattachment of the muscle seems straightforward it can be a frequent source of tightness and stiffness of the chin particularly in sliding genioplasty surgery.
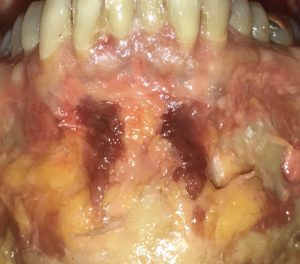
The interesting question is what role does this fat play in mentalis muscle function and what does it mean for surgical manipulation? Functionally it can be presumed to allow the two sides of the muscle to work independently. It allows them to do so without getting ‘stuck’ to each other. It is also likely that the origin of central chin dimples and vertical chin clefts relates to the split of the muscle going more inferiorly and/or the amount of fat between the two split muscles to be less down over the soft tissue chin pad.
From a surgical manipulation standpoint preservation of a broad band of muscle on each side is needed since the central region is just fat…which is unable to hold sutures as a reattachment point. But it also speaks to the treatment of the tight or contracted chin after a sliding genioplasty. Changing the bony anatomy creates the potential for muscle tightness since the length of the mentalis muscle is stretched in advancements, can become tethered down into the newly created bony step deformity and can become tight due to the way the sutures are placed for its reattachment.
Correction of such chin tightness would indicate the need for release and placement of an interpositional fat graft. This would anatomically replicate the need for increased fat volume to fill the ‘space’ left by the lengthening of the bone.
Dr. Barry Eppley
Indianapolis, Indiana