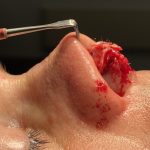
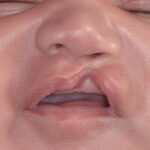
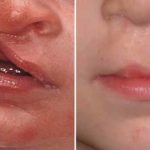
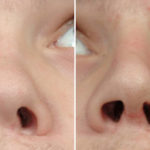
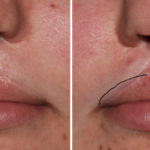
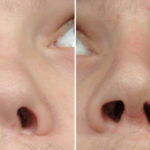
Plastic Surgery Case Study – Secondary Nostril Narrowing and Upper Lip Augmentation in Bilateral Cleft Deformity in a Child

Background: One of the most common congenital facial deformities is that of cleft lip and palate. While occurring in a diverse spectrum of presentations, at the most simplistic level cleft facial deformities can be divided into unilateral and bilateral clefts. What separates the bilateral cleft from unilateral ones is that the central lip segment (prolabium) Read More…