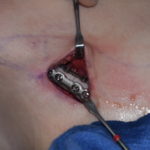
Plastic Surgery Product Review – Refine Soft Tissue Suspension System
The ideal youthful breast has fullness in the upper pole, does not sag, and has a slightly pendulous lower pole. The slope of the upper pole should be slightly convex, straight, or slightly concave. With time, and gravity, many women lose that nice fullness in the upper pole, aging the breast and making it less Read More…