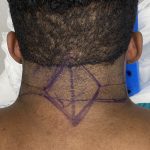
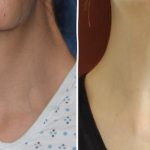
Long-Term Results of the Older Male Direct Neck Lift – Case Study
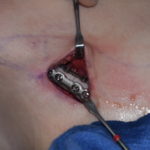
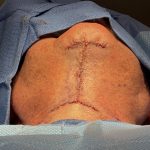
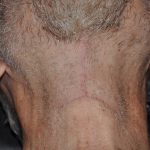
Introduction A direct neck lift is a surgical procedure designed to correct significant neck skin laxity by directly excising excess skin from the anterior neck, rather than relying on indirect skin tightening through a facelift approach. What It Is Excess skin is excised directly from the front of the neck The incision is typically placed Read More…