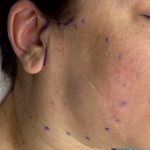
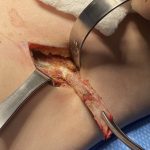
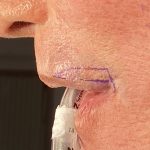
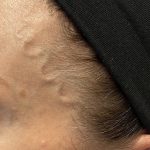
OR Snapshots – Lateral Vermilion Advancements for Improving Upper Lip Shape
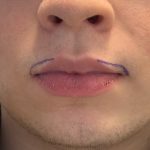
The shape and size of the lips has great variability amongst individuals. Each set of lips is so unique that ‘lip prints’ are almost as individualized as finger prints. There is a natural difference in shape between the upper and lower lips due to the presence of the cupid’s bow in the upper lip which Read More…