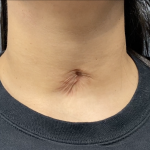
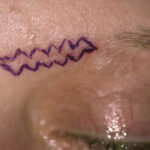
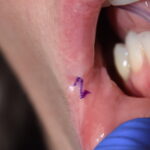
Plastic Surgery Case Study – Female Submentoplasty Scar Revision
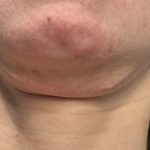
Background: The submentoplasty procedure can be done by a variety of techniques. But what they all share is the need for a skin incisions. This can be a small nick incision right under the chin for liposuction to an elongated inverted T-shaped excision for a direct necklift. But the most common submentoplasty scar is a Read More…