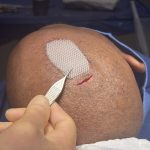
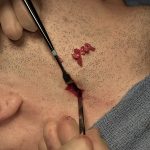
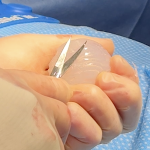
Techniques in Occipital Knob Skull Reduction
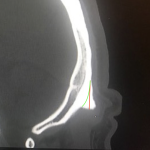
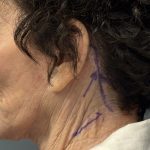
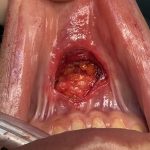
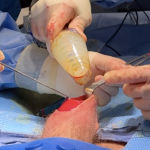
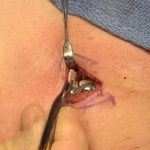
The occipital knob is a well known aesthetic skull deformity which falls into the category of more minor aesthetic skull reshaping surgery. It is easily recognizable as a midline protrusion on the back of the head at the lower end of the visible occipital bone. While it presents with varying degrees of severity it always Read More…