Background: Traumatic loss of part or all of one’s ear at any age poses a difficult reconstructive challenge. In some cases the use of autologous grafts (rib grafts and flaps) can be done. While effective this places an additional vertical scar in the temporal region for flap harvest. This may also be more additional scar that the patient wants to avoid and involves the need for a rib graft harvest as well. In this situation a prosthetic ear reconstruction is the lone remaining option.
A prosthetic ear reconstruction has the advantages of not creating additional scars around the ears and avoiding graft harvests. It also offers the best aesthetic result as it provides the best anatomic match to he opposite ear. But it has several disadvantages including it is not an autologous body part, instability of the ear prosthesis on the flat side of the head and the need to periodically make prosthetic replacements as their colors fade over time with exposure to the sun and weather elements.
Making an ear prosthesis more stable on the side of the head has been solved now for several decades. Borrowing from the concept of dental implants, titanium threaded cylinders are placed in the temporal bone. When healed, they serve as anchoring points to which the the ear prosthesis can ultimately be attached through a mechanical or magnetic mechanism.
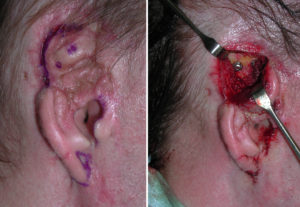
Case Study: This young man suffered a severe dog bite injury to the right side of his head resulting in loss of a portion of his right ear. This resulted in multiple scars and skin grafts around the ear with only the external auditory canal, tragus and a portion of the lower helix and earlobe that remained. Given his traumatic history and need for multiple prior reconstructive surgeries, he was not interested in adding additional scars to the side of his head, having graft harvests or sustaining further complex reconstructive surgeries.

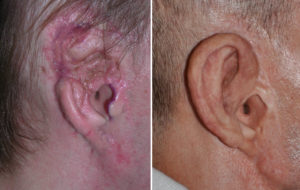
Most ear reconstructions are done with autologous tissues for a natural long-term result. But in adults where the overlying skin quality is damaged by prior trauma, the concept of a total ear reconstruction using either a rib graft or a synthetic framework needs to be considered. The key is the TPF flap harvested from above to cover the ear framework. But some patients may not prefer to go through an autologous reconstructive process and a prosthetic ear is always an option. The use of endosseous implants makes the biggest problem with a prosthesis largely solve.
Highlights:
1) When autologous methods of ear reconstruction are not possible, only a prosthetic ear reconstruction method can be done.
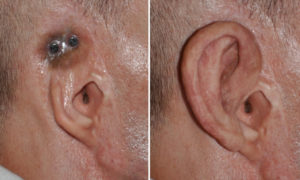
2) To enable more secure anchorage of an ear prosthesis, a bone-anchored method using endosseous implants is used.
3) For good long-term maintenance around the implants a skin graft can be done for a tight soft tissue collar around it.
Dr. Barry Eppley
Indianapolis, Indiana