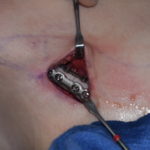
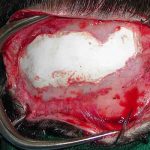
Plastic Surgery Case Study – Split-Thickness Cranial Bone Graft Reconstruction Of Skull Defect
Background: Skull defects can be reconstructed by a variety of methods from implants to grafts. If the patient prefers an autologous method then a bone graft is needed. Technically a bone graft could be obtained from a tissue bank (cadaveric or allograft bone) or from the patient themselves. But for a truly autologous bone graft Read More…