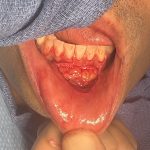
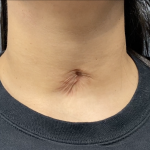
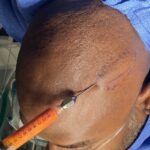
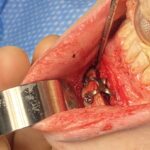
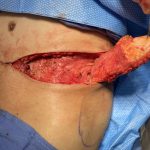
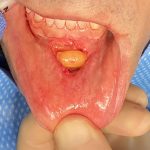
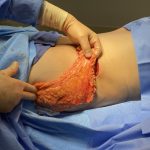
Technical Strategies – Release and Dermal-Fat Grafting in the Treatment of Lower Lip Tightness After A Sliding Genioplasty
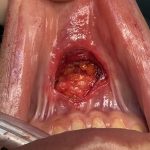
There are a lot of great benefits to a sliding genioplasty chin augmentation procedure but, like all procedures, it has its own unique complications and adverse postoperative sequelae. One of these postoperative issues that can occur is lower lip tightness. Like the upper lip the lower lip is very flexible through the depth of the Read More…