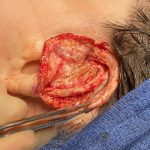
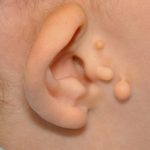
ePTFE-Coated Implant System for Ear Reconstruction
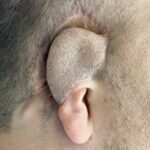
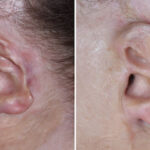
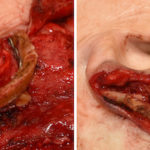
The natural ear is a complex structure consisting of various convexities and concavities. The convexities are the outer helical rim and the Y-shaped superior and inferior crus and antoihelix. The concavities are the large inner most concha around the external auditory canal and the triangular and scaphoid fossas. While the functional significance of these combined Read More…