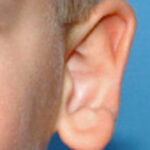
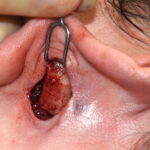
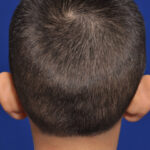
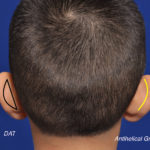
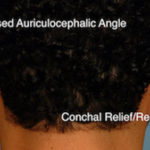
Plastic Surgery Case Study – Secondary Otoplasty Surgery For Maximum Ear Setback
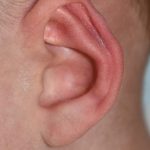
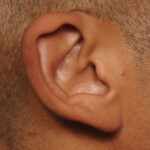
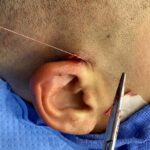
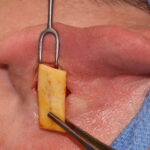
Background: Otoplasty is a very common aesthetic ear surgery that has a long history of various techniques to lessen the appearance of the protruding ear. Regardless of the technique used the goal is to being the ear to a more pleasing position along the side of the head. What the position is has an ideal Read More…