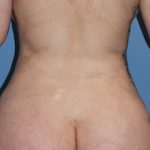
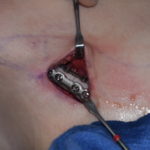
Product Review – Silagen Scar Refinement System
Scars are the result of all elective aesthetic incisions or any method that wounds the skin’s surface. How well any scar will heal depends on a wide variety of factors from its anatomic location, skin thickness, natural degree of pigmentation, and the method that was used to both make the skin injury as well as Read More…